Childhood Routine Immunization in Nigeria: A Call to Action for Community Pharmacists
By Okeke Uchechukwu Chukwudi
Superintendent Pharmacist, Medihub Pharmacare Ltd
Secretary, Association of Community Pharmacists of Nigeria (ACPN), Rivers State Chapter
Introduction
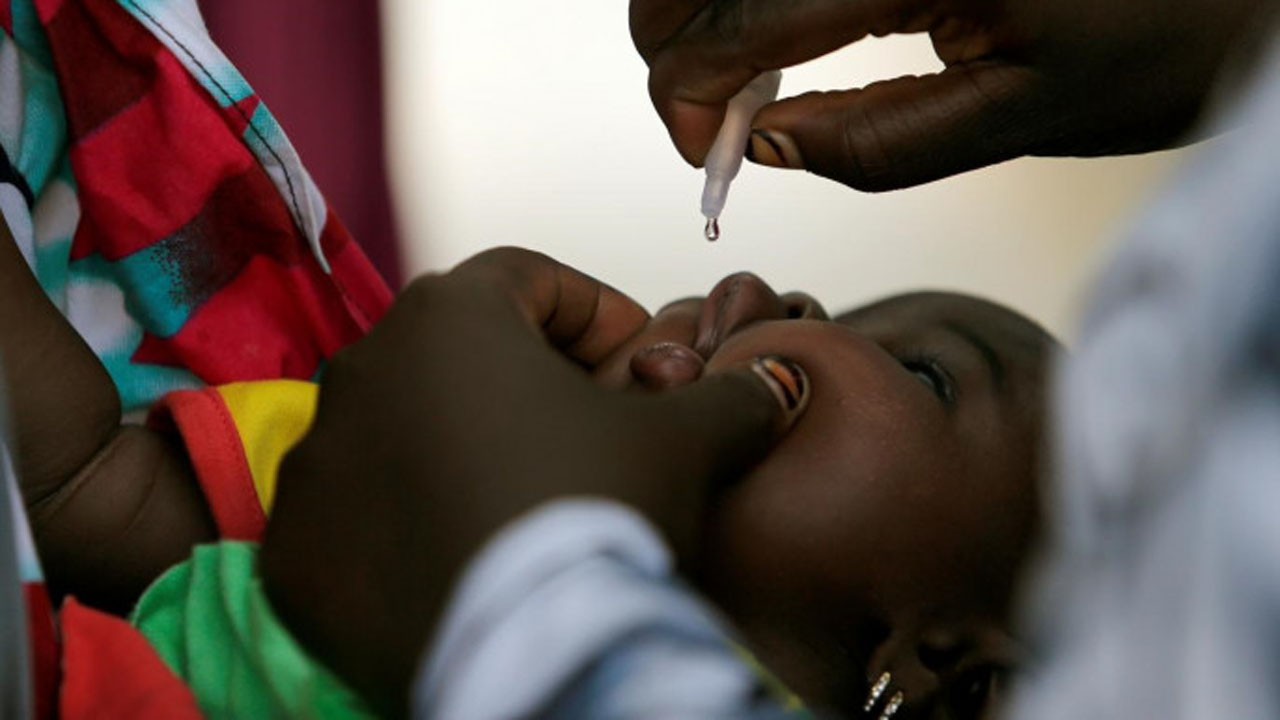
Childhood routine immunization is a cornerstone of public health, significantly reducing morbidity and mortality from vaccine-preventable diseases (VPDs). In Nigeria, the National Programme on Immunization (NPI) aims to provide equitable access to life-saving vaccines for children under five. Despite progress, Nigeria faces persistent challenges, including low coverage rates, logistical barriers, and socio-cultural resistance, resulting in suboptimal protection against VPDs. This article examines the current state of childhood immunization in Nigeria, presents the routine immunization schedule, and explores barriers and strategies for improvement, drawing on recent scientific literature (2015–2025). Recommendations include strengthening health systems, enhancing community engagement, and leveraging technology to improve vaccine delivery.
The Importance of Immunization in Public Health
Vaccination is one of the most cost-effective public health interventions, preventing approximately six million deaths annually from diseases such as measles, polio, and pneumococcal infections (World Health Organization [WHO], 2025). In Nigeria, the Expanded Programme on Immunization (EPI), adopted in 1978, forms the backbone of the NPI, targeting diseases including tuberculosis, diphtheria, pertussis, tetanus, poliomyelitis, and measles. The latest (2021) immunization rate of 76.4% falls below the IA2030 target, and certain socio-economic and sociodemographic factors such as maternal education and geopolitical zone were significantly associated with lower odds of childhood immunization. (Olufadewa et al., 2024). This underscores the urgent need to assess and improve the immunization framework in Nigeria.
Routine Immunization Schedule in Nigeria
The current NPI schedule, aligned with WHO’s EPI, targets children from birth to 18 months and includes recently introduced vaccines such as the pneumococcal conjugate vaccine (PCV) and rotavirus vaccine. The schedule is designed to provide timely protection against 12 vaccine-preventable diseases.
Table 1: Routine Immunization Schedule for Children in Nigeria
| Age | Vaccines Administered | Route | Target Disease(s) |
| At birth | BCG, Hepatitis B (HepB-0), Oral Polio Vaccine (OPV-0) | Intramuscular, Oral | Tuberculosis, Hepatitis B, Poliomyelitis |
| 6 weeks | Pentavalent (DTP-HepB-Hib), PCV-1, Rotavirus-1, OPV-1 | Intramuscular, Oral | Diphtheria, Tetanus, Pertussis, Hepatitis B, Haemophilus influenzae type b, Pneumococcal disease, Rotavirus, Poliomyelitis |
| 10 weeks | Pentavalent-2, PCV-2, Rotavirus-2, OPV-2 | Intramuscular, Oral | Same as 6 weeks |
| 14 weeks | Pentavalent-3, PCV-3, OPV-3, Inactivated Polio Vaccine (IPV) | Intramuscular, Oral | Same as 6 weeks, Poliomyelitis |
| 6 months | Vitamin A (first dose) | Oral | Vitamin A deficiency |
| 9 months | Measles-1, Yellow Fever, Meningococcal A (MenA) | Intramuscular | Measles, Yellow Fever, Meningitis |
| 12 months | Vitamin A (second dose) | Oral | Vitamin A deficiency |
| 15–18 months | Measles-2 | Intramuscular | Measles |
Adapted from Paediatric Association of Nigeria (2020) and WHO (2023).
Current Coverage and Regional Disparities
Recent studies reveal significant coverage gaps and low rates of timely vaccination. A 2025 cross-sectional study in Ebonyi State reported that only 47.2% of children aged 5–11 months had received all vaccines by 14 weeks, and just 8.6% received them on time (Omale et al., 2025). Nationwide, the figure remains low at 34.4%, with stark disparities: South-South region reports 51.5% coverage while the North-West lags at just 9.5% (Davies et al., 2017).
Barriers to Effective Immunization
Several factors hinder optimal vaccine coverage in Nigeria:
- Health System Challenges: Inadequate vaccine supply, frequent stockouts, weak cold chain systems, and insufficient funding and workforce are major issues (Paediatric Association of Nigeria, 2020).
- Socio-Cultural Resistance: Misconceptions, including beliefs that vaccines cause infertility or are unnecessary after polio immunization, are widespread in certain regions. In Kano State, 9.2% of mothers expressed vaccine hesitancy (Ophori et al., 2023).
- Access and Equity: Rural and underserved communities face logistical challenges, while low maternal education and poverty further impede immunization.
- Security Issues: Insurgency in the North-East disrupts immunization efforts, leaving millions of children unvaccinated (Davies et al., 2017).
Infant Mortality Rates: Nigeria vs. Countries with Pharmacist-Led Vaccination
Nigeria’s IMR is notably high at 59.1 per 1,000 live births, driven by low vaccination coverage (34.4%), weak healthcare infrastructure, and socioeconomic barriers (Adeniji & Oyeyemi, 2020). In contrast, high-income countries with pharmacist-led vaccination programs report significantly lower IMR:
- United States: IMR of 5.6 per 1,000, supported by widespread pharmacist-administered vaccines and >90% coverage (Emanuel et al., 2020).
- United Kingdom: IMR of 3.9 per 1,000, with pharmacists delivering flu and other vaccines, contributing to robust systems (Adeniji & Oyeyemi, 2020).
- France: IMR of 3.8 per 1,000, driven by comprehensive child health programs (Dutton, 2021).
- In low- and middle-income settings, India’s Empowered Action Group (EAG) states report IMR of 40–50 per 1,000, reduced through targeted interventions (Roy, 2021). Brazil’s Amazon region has an IMR of 16.6, impacted by environmental and access challenges (Lima et al., 2023).
Pathways to Improvement
Despite these challenges, the introduction of PCV and rotavirus vaccines has significantly reduced related morbidity. However, the WHO’s target of 90% national coverage remains unmet. Addressing the issues of coverage and timeliness requires multi-faceted strategies:
- Strengthening Health Systems: Investments in infrastructure, timely procurement, health worker training, and implementation of strategies like Reaching Every District (RED) have shown promise (Davies et al., 2017).
- Community Engagement: Effective educational campaigns, particularly involving religious and traditional leaders, can improve vaccine acceptance. Community dialogues in northern Nigeria have yielded positive outcomes (Ophori et al., 2023).
- Role of Community Pharmacists: Community pharmacists, often trusted and accessible providers, can play a critical role by offering vaccine education, addressing parental concerns, and serving as referral points. A 2016 study in Lagos found 84.2% of community pharmacies stocked and sold vaccines and possessed necessary storage facilities (Oluwadamilola et al., 2016). Training pharmacists to administer vaccines, as seen in other countries, could improve access, especially in underserved regions.
- Technology and Innovation: Tools like SMS reminders and mobile apps have improved schedule adherence in urban centers (Omale et al., 2025).
- Policy and Advocacy: Enhanced government commitment, strategic partnerships with global health organizations, and policy reforms are essential to bridge funding and operational gaps (WHO, 2025).
Conclusion
Childhood routine immunization in Nigeria remains a critical public health challenge. The current NPI schedule targets major VPDs but suffers from low coverage and poor timeliness. Addressing these issues requires health system reforms, community mobilization, technological support, and the inclusion of community pharmacists in immunization delivery. With strategic planning and collective effort, Nigeria can achieve universal immunization coverage and significantly reduce childhood mortality.
References
- Olufadewa, I., Adesina, M., Oladele, R. et al. Trends and predictors of full immunization coverage in Nigeria. Discov Public Health 21, 151 (2024). https://doi.org/10.1186/s12982-024-00283-x
- Oluwadamilola, F., & Bolajoko, A. (2016). Immunization Services: Involvement of Community Pharmacies in Lagos State, Nigeria. Journal of Pharmaceutical Research International, 12(6), 1–12. https://doi.org/10.9734/BJPR/2016/27442
- Omale, U. I., Ikegwuonu, C. O., Nkwo, G. E., Iwegbulam, C. C., Ekwuazi, L. C., Amuzie, C. I., & Ewah, R. L. (2025). An analytical cross-sectional study on optimal (timely or cumulative age-appropriate) routine childhood immunization coverage in the communities of Ebonyi state, Nigeria. Scientific Reports, 15(1), 3760. https://doi.org/10.1038/s41598-025-87186-2
- Ophori, E. A., Tula, M. Y., Azih, A. V., Okojie, R., & Ikpo, P. E. (2023). Current trends of immunization in Nigeria: Prospect and challenges. Tropical Medicine and Health, 42(2), 67–75. https://doi.org/10.2149/tmh.2013-13
- Paediatric Association of Nigeria. (2020). Immunisation homepage. Paediatric Association of Nigeria. https://pan-ng.org
- World Health Organization. (2023). WHO recommendations for routine immunization – summary tables. https://www.who.int
- World Health Organization. (2025). Vaccines and immunization. https://www.who.int
- Adeniji T, Oyeyemi AY. A Review-Based Comparative Analysis of Health Care Delivery System in Nigeria and the United Kingdom. West Afr J Med. 2020 Nov;37(6):597-605. PMID: 33185253.
- Emanuel EJ, Gudbranson E, Van Parys J, Gørtz M, Helgeland J, Skinner J. Comparing Health Outcomes of Privileged US Citizens With Those of Average Residents of Other Developed Countries. JAMA Intern Med. 2021 Mar 1;181(3):339-344. doi: 10.1001/jamainternmed.2020.7484. PMID: 33369633; PMCID: PMC7770612.
- Dutton, P. V. (2021). Beyond medicine: Why European social democracies enjoy better health outcomes than the United States. Cornell University Press. https://doi.org/10.1215/03616878-10171132
- Roy, M. (2021). Infant mortality in Empowered Action Group States in India: An analysis of sociodemographic factors. Journal of Dr. NTR University of Health Sciences, 10(4), 223–229.
- Lima NRO, Oliveira BFA, Silveira IHD, Oliveira IN, Sousa RFV, Ignotti E. Health in the Legal Amazon: an analysis of morbidity and mortality indicators between 2010 e 2021. Cien Saude Colet. 2025 Jan;30(1):e03722023. doi: 10.1590/1413-81232025301.03722023. Epub 2023 Nov 9. PMID: 39879444.